Basion-axial Interval (BAI)
One of the key measurements used by doctors to assess the stability of the upper neck, is basion-axial interval (BAI.) BAI shows whether the skull is properly aligned with the second cervical vertebra (C2). Sometimes the skull can shift too far forward or backward compared to C2 vertebrae, and it may indicate instability which can put pressure on the brainstem or upper spinal cord.
Traditional radiology imaging looks at BAI in neutral position, however more advanced imaging looks at BAI in a dynamic fashion, specifically in neck flexion and extension. This radiology measurement is called Translational BAI. Often, imaging in neutral can appear normal or borderline, however dynamic imaging is an excellent method to assess whether the skull is properly aligned with C2 in upright and flexion and extension positions.
Both BAI and Translational BAI measurements assess craniocervical instability (CCI), with translational BAI being a newer, advanced radiology measurement.
What part of my body can the basion-axial interval (BAI) be found?
Generally speaking, basion-axial interval (BAI) is a measurement radiologists can use to detect atlanto-occipital dissociation (where the head and neck become unstable).
The basion-atlas interval (BAI) is the distance between two points in your neck: the basion and the posterior arch of the atlas. Doctors use this measurement to check for injuries in the neck area. The basion is a point at the base of your skull, and the atlas is the first cervical vertebra in your neck. Basion-axial Interval (BAI) helps to rule out horizontal atlanto-occipital instability.
How do Radiologists measure BAI?
Radiographical investigations such as X-rays and CT scans are used to measure this. These same tests are used when there is suspicion of any abnormality of the BAI (FIGURE 1).
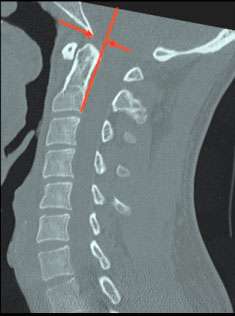
BAI is the distance (in mm) between the basion and the superior extension of the posterior cortical margin of the body of the axis in the median (midsagittal) plane.
What is considered normal BAI for a person?
BAI is considered abnormal when there is anterior displacement of 12 mm or more, or posterior displacement of 4 mm or more, between the basion and posterior C2 line.
What can disturb the regular basion-dens interval?
Any condition causing atlanto-occipital dissociation can also affect the BAI. Atlanto-occipital dissociation injuries are serious injuries that can happen at the joint between the base of the skull and the first vertebra in the neck. These injuries can cause the joint to become unstable because they damage the ligaments that hold it together. This instability can affect the BAI measurement.
What are common symptoms of people with an abnormal BAI?
An abnormality of the BAI, patients could experience the following symptoms:
-
-
- Motor or sensory neurological deficiencies: This can include weakness or loss of sensation in the arms or legs.
- Cranial nerve deficiencies: This can affect vision, hearing, and facial movements.
- Cervical-medullary syndrome: This can cause various symptoms, such as difficulty swallowing, hoarseness, and weakness in the arms or legs.
-
Diagnostic Imaging
Standard anteroposterior, lateral and open-mouth odontoid views as well as flexion and extension are the routine preliminary screening radiographs (XRays).
For many years CT has remained the standard radiologic technique for the craniocervical region. CT with 1 mm slices, and reformatting in both the coronal and sagittal planes provides detailed visualization of the bony relationships and congruency of the atlanto-occipital joints.
Some upper cervical chiropractic clinics utilize CBCT imaging in-office which may be a more easily accessible option than a CT Scan for some patients.
MRI is emerging as a valuable modality in conjunction with CBCT/CT in the diagnosis of atlanto-occipital injuries. MRI is unsurpassed in evaluating neural structures and soft tissues.
Dynamic Imaging and Translational BAI
When investigating craniocervical junction abnormalities, it’s best to seek dynamic imaging in flexion and extension, and if possible, in upright position, to assess for dynamic compression of the brainstem and spinal cord.
Translational BAI is an emerging tool, although it is not widely practiced or recognized and more studies are needed. Reference 1. Reference 2. Recent studies suggest that excessive motion of greater than 2 mm between positions may reflect instability.
Translational BAI Reference Value Guidelines:
Normal is equal or less than 1 mm change between flexion and extension
Borderline abnormal is greater than 2 mm to 4 mm, however clinical correlation is needed.
Abnormal and possible instability is greater than 4 mm change between flexion and extension, especially if symptomatic.
More research is needed in the dynamic translational measurements of BAI.
Is research still active for this BAI?
Because the BAI is due mainly to atlanto-occipital dissociation, which can include dislocation and subluxation, multiple research papers have been conducted on the subject. However, most of these are case studies and are regarded as third place regarding the level of evidence.

BAI REFERENCES
- Hacking C. Basion-axial interval | Radiology Reference Article | Radiopaedia.org [Internet]. Radiopaedia. [cited 2023 Apr 30]. Available from: https://radiopaedia.org/articles/basion-axial-interval-1
- Hosalkar HS, Cain EL, Horn D, Chin KR, Dormans JP, Drummond DS. Traumatic atlanto-occipital dislocation in children. J Bone Joint Surg Am. 2005 Nov;87(11):2480–8.
- Vachata P, Bolcha M, Lodin J, Sameš M. Atlanto-occipital dissociation. Rozhl V Chir Mesicnik Ceskoslovenske Chir Spolecnosti. 2020;99(1):22–8.
- Atlanto-axial instability (AAI): What you need to know [Internet]. Massachusetts General Hospital. [cited 2023 Apr 30]. Available from: https://www.massgeneral.org/children/down-syndrome/atlantoaxial-instability-aai
- Holy M, Szigethy L, Joelson A, Olerud C. A Novel Treatment of Pediatric Atlanto-Occipital Dislocation with Nonfusion Using Muscle-Preserving Temporary Internal Fixation of C0-C2: Case Series and Technical Note. Journal of Neurological Surgery Reports. 2023 Jan;84(01):e11-6.
- Lepard JR, Reed LA, Theiss SM, Rajaram SR. Unilateral atlantooccipital injury: A case series and detailed radiographic description. Journal of Craniovertebral Junction and Spine. 2022 Jul 1;13(3):344.
- Wathen C, Ghenbot Y, Chauhan D, Schuster J, Petrov D. Management of Traumatic Atlantooccipital Dissociation at a Level 1 Trauma Center: A Retrospective Case Series. World Neurosurgery. 2023 Feb 1;170:e264-70.
- García-Pérez D, Panero I, Lagares A, Gómez PA, Alén JF, Paredes I. atlanto-occipital dislocation with concomitant severe traumatic brain injury: A retrospective study at a level 1 trauma centre. Neurocirugía (English Edition). 2023 Jan 1;34(1):12-21.
-
Craniocervical Instability in Ehlers-Danlos Syndrome-A Systematic Review of Diagnostic and Surgical Treatment Criteria.
-
The Association Between Radiographic and MRI Cervical Spine Parameters in Patients With Down Syndrome.


